
This reduces manual workload, accelerates payment cycles, and improves overall efficiency. In-house billing offers more control but requires investment in software, staff training, and dedicated personnel, ideal for small clinics with limited billing volume. Outsourcing reduces administrative workload, provides specialized expertise, and scales efficiently for high-volume or multi-location practices. The decision hinges on cost, internal resources, and workflow complexity.
Visit Details and Service Documentation
In addition to basic identification, the superbill may include provider credentials, tax ID number, and any relevant group affiliation to further support claim validation and reimbursement accuracy. This process can take anywhere from a few hours to several weeks, and delays are common. In fact, 33% of physicians report that the prior authorization process has led to a serious adverse event for a patient in their care due to delays. We deliver accurate cash projections using historical billing data, payer behavior, and consolidated billing trends. This helps facilities anticipate revenue timing and manage financial planning with greater confidence.
What is the Medical Billing Process and How Can You Improve It?

This leads to quick claim payouts and less follow-up from the clinic, as well as less revenue loss. Without proper orthopedic insurance authorization, even correctly coded claims can be denied outright. Behavioral and mental health telehealth services are permanently exempt from geographic restrictions. You can use POS 10 for these visits regardless of where the patient lives.
APCs (Ambulatory Payment Classifications)

Payers often compare revenue codes with bookkeeping for cleaning business procedure codes and place of service details. Any mismatch raises red flags and may result in reduced payment or full claim rejection. Revenue codes are primarily used by hospitals and facility-based providers, but they also apply to outpatient departments, ambulatory surgery centers, and certain institutional healthcare settings.
However, when you do hear from them in the future, make sure your front office team confirms their most recent records. This way, you can easily fix outdated contact and insurance information. Confirm coverage limits, rental caps, and quantity restrictions. Together, these lay the groundwork to provide consumers with protection against surprise billing. Stand out from the competition with a template specifically optimized for applicant tracking systems. Try this resume template — Last month, 158 job seekers landed interviews at top companies using our professionally-designed resume template.

Capture complete and up-to-date demographic, insurance, and https://www.bookstime.com/ contact information before every visit. When claims are accurate and timely, your practice can count on reimbursements arriving as expected. Your admin team will be bogged down with tedious work, and patient satisfaction is going to suffer. Colloquially, prior authorization for orthopaedics is payer permission to perform specific orthopaedic surgical, imaging, or therapeutic procedures prior to delivery.
CPT® code set overview
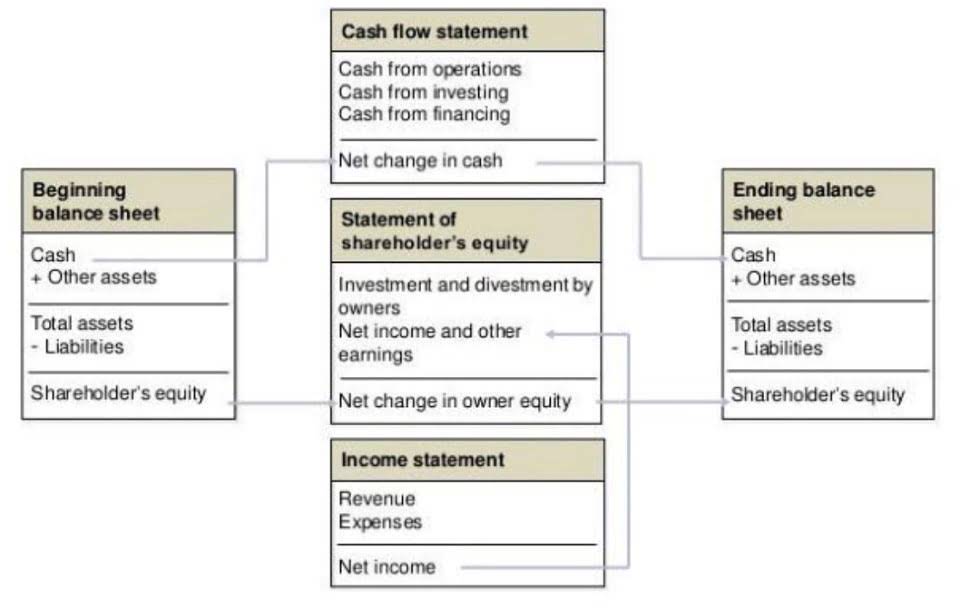
By tracking key metrics, a practice can monitor the performance of its revenue cycle and find opportunities to improve. Once the claim has been created, coded, and scrubbed, it is submitted to the insurance company for reimbursement. This is the point where the clinical service is documented for billing purposes. During the visit, the physician records all diagnoses made and procedures performed in the patient’s medical record. Of course, even if your claims are squeaky clean, insurers can deny them. In this case, your billing team should review the payer’s decision, which will often be detailed, for potential inaccuracies.
- National billing companies often route client communications through call centers staffed by representatives who lack direct knowledge of your account.
- Imagine receiving home medical equipment from your HME provider—perhaps a CPAP machine, a wheelchair, or oxygen therapy supplies.
- The operational activities of hospitals rely on medical billing, which serves as a vital yet intricate component of their work.
- Developed by the American Medical Association (AMA), they standardize how services are reported across healthcare providers and insurers.
- Small errors in names, policy numbers, or dates create denial risks later.
When contracts fall below market norms, your billing partner provides the data and analysis needed to negotiate better terms. Effective patient billing balances the need for timely payment with sensitivity to patients’ financial situations. Local experts medical billing process understand the economic realities of your community and can tailor collection efforts accordingly. They maintain professional yet compassionate communication that preserves patient relationships while improving payment performance. Local auditors can conduct onsite reviews that include provider education and real-time feedback.








Recent Comments